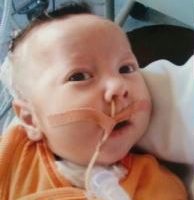
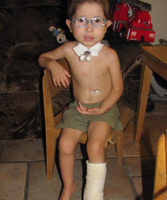
Casey is a 12-year-old girl who suffered from severe multilevel laryngotracheal stenosis and a tracheostomy since a long time. She had undergone several endoscopic and open operations in the past in the UK. Dr Sandu was invited to perform an extended cricotracheal resection surgery at the Alder Hey children’s hospital, Liverpool. Following this surgery and a successful decannulation – that is removal of the tracheostomy cannula, she has had an excellent outcome and is making tremendous progress at school and in her daily life. She is seen here with her family.
Patient reviews
INPAF
Casey
HUMANITARIAN SERVICES IN LOW RESOURCE SETTINGS
Dr Sandu has performed more than 100 successful airway operations in children and adults in Morocco, Algeria, Iran, India, Sri Lanka and Chile.
I am text block. Click edit button to change this text. Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
Roosi-Mai
Our daughter Roosi-Mai was one and a half years old when she swallowed a button battery.
At the beginning it seemed that the situation wasn´t that bad but the reality was something else.
Life of our family changed completely.
We lived almost half a year in a hospital in the intensive care unit. She could not eat and drink at all. Her foodpipe was totally closed and there was a tunnel between airpipe and foodpipe.
We fed our daughter through a central vein and also through a g-tube to the stomach.
The first surgery was in Estonian hospital in Tallinn, but as she had complex injuries in foodpipe and trachea, her problems couldn’t be solved here.
The doctors team in Estonian had had cooperation with Dr Kishore Sandu in CHUV before, so our they decided to send Roosi-Mai to CHUV in Switzerland to treat her there.
Dr Sandu explained that our problems are complex and three things have to be solved with one surgery.
The surgery was done in November and it went well. It changed everything.
Our little daughter could start to eat, drink and breathe again normally.
Our home doesn’t look like hospital anymore.
We can live normal life and our Roosi-Mai is three year old happy girl.
It’s not insignificant that Estonian health care system has covered all medical costs.
There are not enough words to describe our gratefulness to Dr Sandu, other doctors and all the team in CHUV. They make a wonderful work that really changes the world.
Thelma
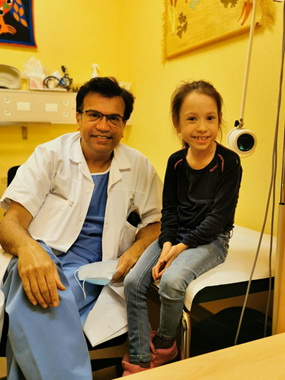
THELMA was referred from Norway with severe multilevel laryngotracheal stenosis. Here, she is seen with Dr Sandu after her successful surgery.

Paolo
Paolo lives in Greece and suffered from severe sequelae (a very large tracheoesophageal fistula) after an intubation for COVID infection. He is seen with his doctor, Prof Hatziagorou after a successful treatment.

Camilla
Camilla was referred from Italy and had severe stenosis of her trachea following surgery for congenital malformations of the food and windpipes. In the past, she had undergone several operations. Here, she is seen at her home after an excellent recovery following treatment in Lausanne.

Andreas
Andreas was born with congenital paralysis of his vocal cords, and had tracheostomy in early months of his life. He was successfully decannulated and continues to grow like a normal child.


Paul
Annette
Annette, 55 years, was diagnosed to have severe degree of idiopathic subglottic stenosis. She used to get tired walking just a small distance. It was getting impossible for her to carry-on with daily day to day household work.
She underwent a single-stage cricotracheal resection. She now leads a normal life and loves hiking up the mountains and skiing.
Malena
Malena had undergone an extensive thoracic surgery for a congenital lung malformation at 6 months of age. She had a tracheostomy immediately after the surgery, followed by development of severe grade of subglottic stenosis.
She underwent a cricotracheal resection with excision of 6 tracheal rings, the subglottis and the tracheostomy – all in a single operation.
The Weibel family seen 3 months later during the check endoscopy which showed complete healing of the operation site.
Here, we see Malena enjoying the snow with her elder sister two and half months after the surgery at the Lausanne University Hospital.
Matilde
Matilde, a 2-year old girl was referred from Portugal to our institution. She is a case of Pierre Robin sequence and had a tracheostomy when she was 19 days old for severe grade IV subglottic stenosis. She acquired the airway stenosis following repeated intubations. Ever since, she had several episodes of hospitalizations for multi-resistant lung infections. She was referred to the CHUV for further treatment. When Matilde arrived at the CHUV – she had a tracheostomy and produced no voice. Matilde underwent a cricotracheal resection and now leads a normal life – without a tracheostomy, eats and drinks and plays normally and has a communicable voice.
Zaccharia
Zacharria is a 3-year-old boy living in Helsinki, Finland. He was diagnosed to have a congenital bilateral vocal cord paralysis and had to depend on a tracheostomy to breathe. In 2016, an operation at the University Hospital of Lausanne allowed him to remove the cannula and since then has been living without the tracheotomy. He now enjoys each moment of this new life with his little sister.
Benthe
Benthe was born premature at 28 weeks with a birthweight of 750 grams. She received a tracheostomy at 3 months of age after repeated intubations caused severe stenosis (grade IV) and damage to the vocal cords, leaving her unable to breathe or speak.
At the age of 2 years, she underwent a 2-stage extended cricotracheal resection and anastomosis (EPCTR) including vocal cord correction. Further, she had minor endoscopic procedures and over a period of 6 months after removal of the trachea cannula, she whispered her first words!
Currently, she is a happy 3½ years old (picture) able to speak, eat, drink and play like any other healthy child of her age.
Milena
Aron
Aron suffered from feeding difficulties and severe inspiratory stridor. He was diagnosed to have severe laryngomalacia and underwent a laser treatment.
Here, he is seen 3 months after the surgery with his twin brother and parents. Today, he feeds well, has gained weight and has no breathing problems.
Leon
Leon is a 6-year-old boy from Slovenia who had tracheostomy in early months of his life.
He had a complex single lung condition and a long laryngotracheal cleft- meaning that the food pipe and the air pipe were one and not separated from each other.
He underwent surgery for his cleft in Lausanne and following its success, the tracheostomy was subsequently closed.
Here, we see Leon with his parents who had tears of joy in their eyes to see him without the cannula. The surgery completely changed their quality of life.
Tomasso
Tomasso lives in Italy and had to be intubated immediately after birth for severe prematurity. Unfortunately, his twin brother died some days after their birth. Prolonged endotracheal intubation caused severe multi-site laryngotracheal stenosis that required a tracheostomy. At the CHUV, he underwent an extended cricotracheal resection and following which, the tracheostomy was successfully removed